
Pediatric Hypotonia is a condition characterized by decreased muscle tone that affects infants and children at various stages of development. Muscle tone refers to the amount of resistance muscles have to passive movement, and when tone is low, children may appear floppy or weak. Early identification and intervention play a crucial role in helping children with hypotonia reach their developmental potential. With timely support, many children experience meaningful improvements in movement, posture, coordination, and daily functioning.
This article explores early intervention strategies for children with Pediatric Hypotonia, emphasizing the importance of comprehensive assessment, therapeutic approaches, family involvement, and long term developmental support.
Understanding Pediatric Hypotonia
Pediatric Hypotonia is not a diagnosis on its own but rather a clinical sign that may be associated with a wide range of neurological, genetic, metabolic, or musculoskeletal conditions. In some cases, the cause may remain unknown.
Children with hypotonia often demonstrate delayed motor milestones, poor head control, challenges with balance, and difficulties maintaining posture. These challenges can impact feeding, speech development, mobility, and overall independence if not addressed early.
Importance of Early Intervention
Early intervention refers to therapeutic and developmental services provided during infancy and early childhood. This period is critical because the developing brain has a high level of adaptability. Addressing hypotonia early allows therapists and caregivers to support muscle activation, motor planning, and functional skills before compensatory patterns develop.
Benefits of Early Support
Early intervention for Pediatric Hypotonia offers several benefits.
Improved muscle strength and endurance
Enhanced postural control and balance
Better coordination and movement efficiency
Support for feeding and speech development
Increased confidence and participation in daily activities
Children who receive early therapy often show better long term outcomes compared to those who begin treatment later in childhood.
Early Identification and Assessment
Timely recognition of Pediatric Hypotonia is the foundation of effective intervention. Parents, caregivers, and healthcare providers often notice early signs during infancy.
Common Early Signs
Difficulty lifting or controlling the head
Delayed rolling, sitting, or crawling
Poor tolerance for tummy time
Excessive flexibility or joint laxity
Weak grasp or limited spontaneous movement
When these signs are observed, a comprehensive evaluation is recommended.
Multidisciplinary Evaluation
Assessment typically involves a team approach that may include pediatricians, neurologists, physical therapists, occupational therapists, and speech language specialists. The evaluation focuses on muscle tone, strength, reflexes, coordination, feeding skills, and overall development.
Physical Therapy as a Core Intervention
Physical therapy is often the cornerstone of early intervention for Pediatric Hypotonia. The primary goal is to improve gross motor skills, strength, and postural stability.
Focus Areas in Physical Therapy
Physical therapy sessions emphasize purposeful movement and functional skill development.
Head and trunk control
Weight bearing through arms and legs
Balance and postural reactions
Transitions such as sitting to standing
Gait development and mobility
Therapists use play based activities to encourage active participation and motivation.
Home Exercise Programs
Caregivers are often guided on how to continue therapy activities at home. Consistency across environments helps reinforce skills and accelerates progress.
Occupational Therapy for Functional Development
Occupational therapy supports children with hypotonia by addressing fine motor skills, sensory processing, and daily activities.
Enhancing Fine Motor Skills
Children with Pediatric Hypotonia may struggle with grasping, releasing, and manipulating objects. Occupational therapy focuses on strengthening hands and improving coordination through age appropriate activities.
Sensory Integration Support
Low muscle tone can be associated with sensory processing challenges. Occupational therapy helps children interpret sensory information more effectively, improving body awareness and motor planning.
Daily Living Skills
As children grow, occupational therapy supports independence in tasks such as feeding, dressing, and play participation.
Speech and Feeding Therapy
Hypotonia can affect the muscles involved in feeding and speech. Early involvement of speech language therapy is essential for children showing signs of oral motor weakness.
Feeding Support
Infants with hypotonia may have difficulty sucking, chewing, or swallowing. Therapy focuses on strengthening oral muscles and promoting safe feeding patterns.
Communication Development
Speech therapy also supports language development, sound production, and breath control. Early communication support helps reduce frustration and encourages social interaction.
Role of Orthotic and Adaptive Support
Some children with Pediatric Hypotonia benefit from supportive devices that enhance alignment and stability.
Postural Support
Adaptive seating systems may be used to promote proper posture during play and feeding. Proper alignment reduces fatigue and allows children to engage more fully in activities.
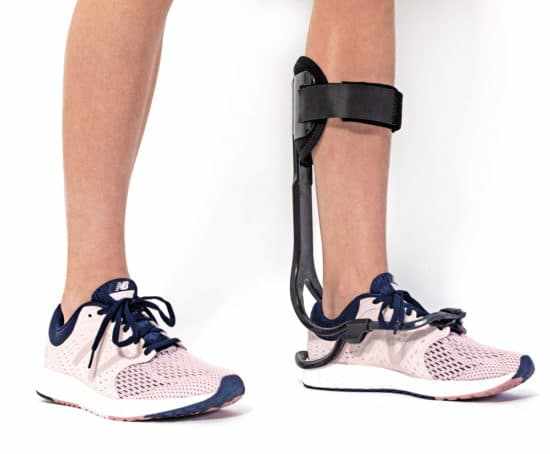
Lower Limb Support
Bracing or supportive footwear may be recommended to improve stability during standing and walking. These supports are typically used alongside therapy rather than as a standalone solution.
Family Involvement and Education
Family involvement is one of the most critical elements of successful early intervention. Caregivers play an active role in supporting development throughout daily routines.
Empowering Caregivers
Education helps families understand Pediatric Hypotonia and how to incorporate therapeutic strategies into everyday activities. Simple adjustments in positioning, play, and handling can make a significant difference.
Emotional Support
Receiving a diagnosis can be overwhelming. Providing emotional support and realistic expectations helps families remain engaged and confident throughout the intervention process.
Monitoring Progress and Adjusting Strategies
Children with hypotonia develop at their own pace, and intervention plans must evolve as needs change.
Ongoing Reassessment
Regular follow up allows therapists to monitor progress, identify emerging challenges, and adjust goals accordingly. As children gain strength and skills, therapy may shift toward higher level coordination and endurance.
Transitioning to School Based Support
As children approach school age, collaboration with educators ensures continuity of care. Early intervention lays the foundation for successful participation in educational and social environments.
Long Term Outlook for Children with Hypotonia
The long term outlook for children with Pediatric Hypotonia varies depending on the underlying cause and the effectiveness of early intervention. Many children make significant gains in strength, coordination, and independence with appropriate support.
Early intervention does not aim to change muscle tone alone but focuses on maximizing functional abilities and quality of life. With the right strategies, children can participate actively in play, learning, and community life.
Conclusion
Early intervention strategies play a vital role in supporting children with Pediatric Hypotonia. Through timely assessment, individualized therapy, family involvement, and consistent follow up, children can achieve meaningful developmental progress. A collaborative approach ensures that physical, functional, and communication needs are addressed during the most critical years of growth. Continued awareness and education help families and professionals work together to create positive outcomes for children with hypotonia.










Write a comment ...