Charcot Neuroarthropathy (CNA) is a complex and often debilitating condition that affects the joints, leading to severe joint deformity and, in some cases, the loss of function. While rare, it is most commonly associated with individuals who have underlying neurological conditions such as diabetes, and it can cause extensive damage if not treated early. In this article, we will explore what Charcot Neuroarthropathy is, its causes, symptoms, diagnosis, and available treatment options. This article will provide a comprehensive guide to understanding and managing this serious health condition.
What is Charcot Neuroarthropathy?
Charcot Neuroarthropathy is a disorder that primarily affects the joints, causing progressive degeneration and deformities. It occurs when there is nerve damage in the affected area, which leads to a loss of sensation and, consequently, a lack of protective responses during joint stress. This results in repetitive trauma and inflammation, which gradually destroys the joint structures.
The condition is most commonly seen in the lower extremities, particularly the feet and ankles, but it can also affect the knees, wrists, and other joints. People with diabetes are particularly vulnerable, as diabetic neuropathy (nerve damage) increases the risk of Charcot Neuroarthropathy.
How Does Charcot Neuroarthropathy Develop?
Charcot Neuroarthropathy develops as a result of a combination of sensory nerve damage and mechanical stress on the joints. When the nerves are damaged, the brain no longer receives the normal sensory feedback about the joint’s position, force, or alignment. Without this critical information, individuals may unknowingly place excessive stress on the affected joint, leading to microfractures, dislocations, and other injuries. Over time, these injuries can lead to severe joint destruction.
The lack of pain or discomfort (due to the loss of sensation) often allows individuals to continue using the affected joint, exacerbating the damage. This process can occur over weeks, months, or even years, depending on the severity of the nerve damage and the individual's activity levels.
Causes and Risk Factors
Charcot Neuroarthropathy can develop for a variety of reasons, but the most common underlying cause is neuropathy, particularly diabetic neuropathy. Neuropathy is a condition that results from nerve damage, which affects the sensation and function of nerves in the body. However, other conditions can also increase the risk of developing CNA.
Diabetic Neuropathy
Diabetes, especially when poorly controlled, can lead to nerve damage in the feet and other parts of the body. The blood vessels supplying the nerves become damaged, impairing the nerves' ability to send signals to the brain. As a result, individuals with diabetes may develop numbness, tingling, or a complete loss of sensation in their extremities. This loss of sensation can make them unaware of joint damage or injury, contributing to the development of Charcot Neuroarthropathy.
Other Causes of Charcot Neuroarthropathy
While diabetes is the leading cause, other factors can contribute to the development of Charcot Neuroarthropathy. These include:
Spinal Cord Injury: Damage to the spinal cord can disrupt nerve function, leading to neuropathy and an increased risk of CNA.
Peripheral Neuropathy: This is any nerve damage affecting the peripheral nervous system, which can occur due to various conditions such as alcoholism, vitamin deficiencies, or autoimmune diseases.
Syringomyelia: A condition in which a cyst or cavity forms within the spinal cord, causing nerve damage and increasing the risk of Charcot Neuroarthropathy.
Other Neurological Disorders: Conditions like multiple sclerosis and Parkinson’s disease that affect the nervous system can also increase the likelihood of developing CNA.
Symptoms of Charcot Neuroarthropathy
The symptoms of Charcot Neuroarthropathy can vary depending on the severity of the condition and the joint(s) involved. However, the primary feature of this disorder is joint destruction without the usual pain that one might expect from such damage.
Early Signs and Symptoms
In the early stages, the symptoms can be subtle and may include:
Swelling: Swelling is one of the first noticeable signs of CNA. It may occur suddenly and can affect the joint area without any obvious injury.
Redness or Heat: The affected joint may appear red or feel warm to the touch due to inflammation.
Instability: The joint may become unstable or loose, making it difficult to walk or bear weight on it.
Advanced Symptoms
As Charcot Neuroarthropathy progresses, the following symptoms may appear:
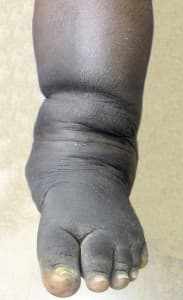
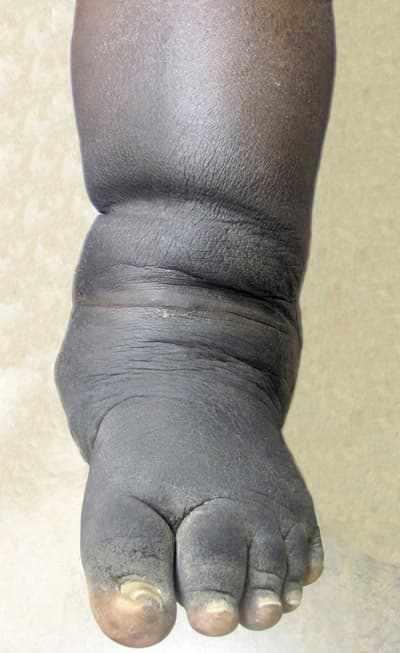
Joint Deformities: The affected joint(s) may begin to deform, with a visible change in shape or alignment. This is often due to the destruction of cartilage, bones, and soft tissues in the joint.
Loss of Function: As the joint deteriorates, individuals may experience a significant loss of mobility or function in the affected area.
Inability to Feel Pain: One of the hallmark signs of CNA is the absence of pain despite extensive damage. This can lead to continued use of the joint, which accelerates the condition’s progression.
Diagnosing Charcot Neuroarthropathy
Diagnosing Charcot Neuroarthropathy can be challenging, particularly because the lack of pain may mask the extent of the joint damage. However, healthcare professionals rely on a combination of clinical evaluation, imaging studies, and a thorough patient history to make a diagnosis.
Clinical Evaluation
The first step in diagnosing CNA is a physical examination, where a doctor will assess the symptoms, including swelling, deformity, and joint instability. The doctor will also evaluate the patient for any underlying conditions like diabetes or neurological disorders that might predispose them to the condition.
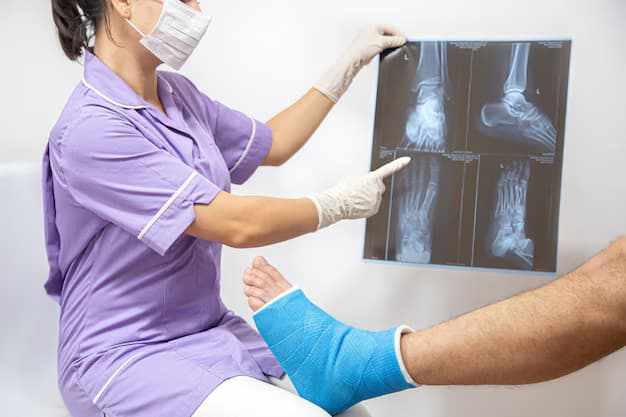
Imaging Studies
X-rays, CT scans, and MRIs are essential tools in diagnosing Charcot Neuroarthropathy. These imaging studies can reveal the extent of joint damage, fractures, and deformities. In some cases, bone scans may also be used to detect inflammation and stress fractures that are not visible on standard imaging.
Treatment of Charcot Neuroarthropathy
Early diagnosis and appropriate management are key to preventing the progression of Charcot Neuroarthropathy and preserving joint function. Treatment generally focuses on alleviating symptoms, preventing further damage, and promoting joint stability.
Conservative Management
In the early stages of CNA, conservative treatments can help control inflammation and protect the affected joint. These include:
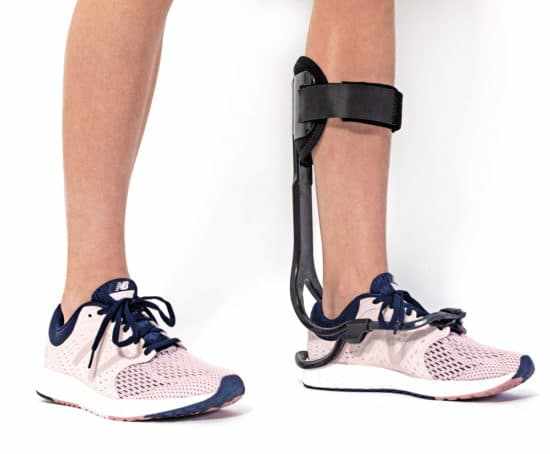
Rest and Immobilization: Resting the joint and using supportive devices like casts, braces, or special footwear can help prevent further stress and allow the joint to heal.
Medications: Anti-inflammatory drugs (NSAIDs) may be prescribed to reduce swelling and pain. However, because pain may not be a significant symptom, anti-inflammatory drugs are used primarily for inflammation control.
Custom Orthotics: Special footwear and insoles can help distribute weight more evenly and relieve pressure on the affected joint.
Surgical Treatment
If the joint damage becomes severe or if the condition leads to significant deformities, surgery may be necessary. Surgical options include:
Joint Fusion: In some cases, doctors may recommend fusing the affected joint to prevent further movement and reduce pain or instability.
Amputation: In extreme cases where the joint is beyond repair and causing significant problems, amputation of the affected limb may be required.
Ongoing Care
Even after the acute phase of the disease has been managed, individuals with Charcot Neuroarthropathy may require long-term care and monitoring. Regular follow-up visits with a healthcare provider, physical therapy to maintain mobility, and adjustments to footwear or orthotics may be necessary to prevent recurrence or further complications.
Conclusion
Charcot Neuroarthropathy is a serious condition that can cause significant joint damage, especially when left untreated. Early detection, appropriate treatment, and management are critical to minimizing long-term disability and improving quality of life. While the condition is complex, advancements in medical care have improved outcomes for many individuals. For those at risk, particularly individuals with diabetes or neurological disorders, it is essential to work closely with healthcare providers to monitor and manage the condition effectively.
For more information and expert advice, visit Ler Magazine.











Write a comment ...