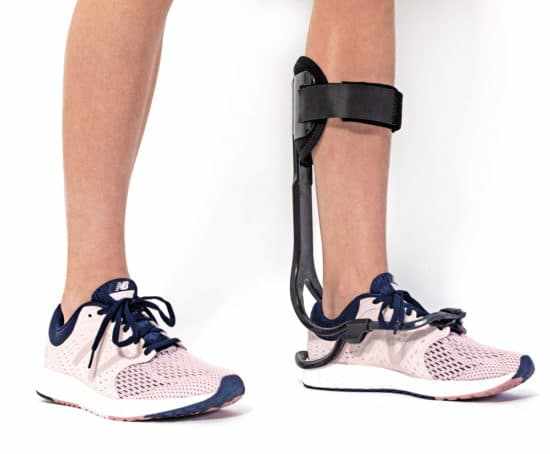
Foot drop is a common movement impairment that affects many individuals following stroke and other neurological conditions. It interferes with the ability to lift the front part of the foot during walking, often leading to instability, compensatory movement patterns, and a higher risk of falls. Effective Management of Foot Drop requires a thorough understanding of its causes, careful assessment, and a coordinated rehabilitation approach tailored to the individual.
This article explores foot drop in the context of stroke and neurological disorders, outlining its causes, assessment, and a wide range of management strategies that support mobility, safety, and quality of life.
Understanding Foot Drop in Neurological Conditions
Foot drop is not a disease itself but a sign of underlying neurological or muscular dysfunction. It results from weakness or paralysis of the muscles responsible for lifting the foot, most notably the ankle dorsiflexors. In neurological conditions, this weakness is often linked to disrupted nerve signals between the brain, spinal cord, and lower limb muscles.
Causes of Foot Drop After Stroke
Stroke is one of the most common causes of foot drop. Damage to motor areas of the brain or the neural pathways controlling the lower limb can reduce voluntary muscle activation. This leads to difficulty lifting the foot during the swing phase of walking. Muscle stiffness, altered reflexes, and poor coordination may further contribute to the problem.
Foot Drop in Other Neurological Disorders
Beyond stroke, foot drop may occur in conditions such as multiple sclerosis, traumatic brain injury, spinal cord injury, and peripheral nerve damage. Each condition affects the nervous system differently, but the resulting impairment in ankle control often presents similar functional challenges.
Impact of Foot Drop on Daily Life
Foot drop can significantly affect mobility and independence. Individuals may adopt compensatory strategies such as lifting the knee excessively or swinging the leg outward to avoid dragging the toes. These adaptations increase energy expenditure and may lead to pain or secondary joint problems over time.
Risk of Falls and Injury
One of the most serious consequences of foot drop is the increased risk of tripping and falling. Reduced toe clearance during walking makes uneven surfaces and stairs particularly hazardous. Falls can result in fractures, fear of movement, and reduced participation in daily activities.
Psychological and Social Effects
Mobility limitations caused by foot drop can also impact emotional wellbeing. Frustration, reduced confidence, and social withdrawal are common, especially when walking becomes slow or visibly altered. Addressing these concerns is an important part of comprehensive management.
Assessment and Diagnosis
Effective management begins with a thorough assessment conducted by a qualified healthcare professional. The goal is to identify the underlying cause, severity, and functional impact of foot drop.
Clinical Examination
A physical examination typically includes evaluation of muscle strength, joint range of motion, reflexes, and walking pattern. Observation of gait provides valuable insight into how foot drop affects movement and balance.
Neurological Evaluation
Neurological assessment helps determine whether foot drop originates from central or peripheral nervous system involvement. Imaging studies and nerve conduction tests may be used when necessary to clarify the diagnosis.
Functional Assessment
Assessing how foot drop affects daily activities such as walking indoors, navigating stairs, and performing self care tasks helps guide treatment planning. Patient goals and lifestyle factors are also considered during this process.
Rehabilitation Based Management Approaches
Rehabilitation plays a central role in improving mobility and reducing the impact of foot drop. Interventions are often combined to address strength, coordination, and functional walking ability.
Therapeutic Exercise Programs
Targeted exercises aim to strengthen weakened muscles and improve motor control. These programs may include ankle dorsiflexion exercises, balance training, and task specific walking practice. Consistency and progression are key to achieving meaningful improvements.
Gait Training and Motor Relearning
Gait training focuses on restoring a more efficient and symmetrical walking pattern. Techniques may involve verbal cues, visual feedback, and repetitive practice to retrain the nervous system. Motor relearning principles emphasize active participation and task relevance.
Stretching and Spasticity Management
In some neurological conditions, muscle tightness and spasticity contribute to foot drop. Gentle stretching and positioning strategies help maintain joint mobility and reduce resistance to movement. Managing muscle tone supports smoother and safer walking.
Assistive and Orthotic Interventions
When muscle weakness persists, external support can enhance stability and function during walking.
Ankle Support Devices
Ankle support devices help maintain the foot in a neutral position during the swing phase of gait. By preventing the toes from dropping, these devices improve toe clearance and reduce the risk of tripping. Proper fitting and regular review are essential to ensure comfort and effectiveness.
Functional Electrical Stimulation
Functional electrical stimulation uses controlled electrical impulses to activate the muscles responsible for lifting the foot during walking. This approach can enhance muscle activation and promote a more natural gait pattern in selected individuals.
Mobility Aids and Environmental Modifications
In some cases, walking aids and home modifications provide additional safety and confidence. Clear pathways, appropriate footwear, and adequate lighting also contribute to fall prevention.
Long Term Management and Recovery
Foot drop management is often an ongoing process, particularly in chronic neurological conditions. Long term success depends on regular monitoring, adaptation of strategies, and active patient involvement.
Importance of Early Intervention
Early identification and treatment of foot drop can prevent secondary complications and support better functional outcomes. Prompt rehabilitation helps maintain muscle activity and encourages optimal movement patterns.
Role of Education and Self Management
Educating individuals and caregivers about foot drop empowers them to participate actively in rehabilitation. Understanding how to use support devices, perform exercises correctly, and recognize changes in function promotes long term independence.
Monitoring Progress and Adjusting Treatment
Regular follow up allows healthcare providers to assess progress and adjust interventions as needed. Changes in strength, walking ability, or overall health may require modifications to the management plan.
Multidisciplinary Approach to Care
Effective foot drop management often involves collaboration among various healthcare professionals. Physiotherapists, occupational therapists, physicians, and rehabilitation specialists each contribute unique expertise.
Coordinated Treatment Planning
A coordinated approach ensures that interventions complement each other and align with the individual goals of the person affected. Communication among team members supports consistent and effective care.
Addressing Whole Person Needs
Beyond physical rehabilitation, comprehensive care considers emotional, social, and environmental factors. Supporting participation in meaningful activities enhances overall quality of life.
Conclusion
Foot drop is a challenging yet manageable condition commonly seen after stroke and in other neurological disorders. Through careful assessment, individualized rehabilitation, and appropriate supportive interventions, many individuals experience improved mobility and confidence. Ongoing education, early intervention, and a multidisciplinary approach are key to successful outcomes. By focusing on functional goals and patient centered care, foot drop management can significantly enhance independence and daily living.
This article is proudly presented by Ler Magazine.











Write a comment ...