Transmetatarsal amputations represent a significant surgical procedure that involves removing the front portion of the foot through the metatarsal bones. Although the surgery is only partial, the outcome profoundly influences balance, gait, and day to day function. Many individuals undergo this procedure due to complications from diabetes, severe infections, traumatic injuries, or vascular conditions that compromise the tissue of the forefoot. Understanding the reasons behind the procedure and the impact on mobility helps individuals, families, and clinicians make informed decisions that support long term recovery and independence.
While transmetatarsal amputations are often viewed as life altering, modern approaches to rehabilitation, prosthetic design, and therapeutic interventions enable individuals to regain considerable mobility. With appropriate care, many people return to walking, recreational activities, and meaningful participation in daily routines.
What Transmetatarsal Amputations Involve

Location and extent of the procedure
A transmetatarsal amputation removes the front portion of the foot through the shafts of the metatarsal bones. This preserves the hindfoot and midfoot, which provides an advantage compared to more proximal amputations. The heel pad remains intact, which allows individuals to continue bearing weight on the back of the foot.
Why this level of amputation is chosen
Surgeons often consider this procedure when the forefoot cannot be saved due to non healing wounds, severe infections, gangrene, traumatic injury, or complications from chronic conditions. The goal is to remove unhealthy tissue while keeping as much functional foot structure as possible.
Functional advantages of retaining the heel
Because the heel remains intact, individuals can continue to place weight through the back of the foot. This structural preservation improves balance, helps maintain a more natural gait pattern, and reduces the amount of prosthetic support required compared to higher level amputations.
Common Conditions Leading to Transmetatarsal Amputations
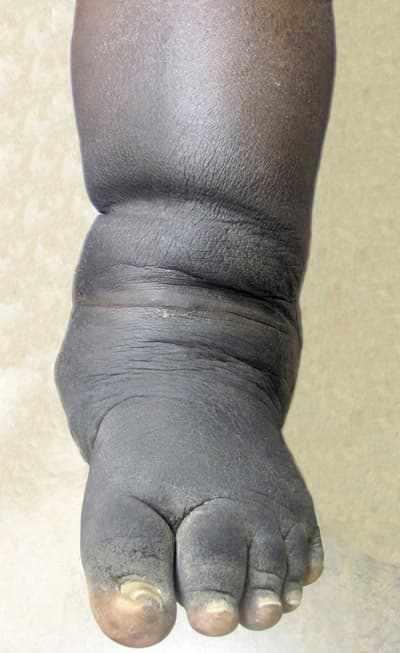
Diabetes related complications
One of the leading causes of transmetatarsal amputations is uncontrolled diabetes. Poor circulation and neuropathy often result in ulcers that do not heal. If infection spreads to deeper structures, amputation may be necessary to prevent further tissue damage.
Severe infections
Infections that extend into the bones or surrounding tissues may require amputation to prevent systemic complications. When conservative treatment fails, removing the affected portion of the foot becomes the safest option.
Traumatic injuries
Accidents involving heavy machinery, crush injuries, or penetrating trauma may damage the forefoot beyond repair. In these cases, transmetatarsal amputations provide a way to preserve remaining function.
Vascular disease
Poor blood flow due to peripheral artery disease can lead to tissue death in the forefoot. When revascularization is not possible or not successful, amputation may be required.
Immediate Postoperative Considerations
Protecting the surgical site
After surgery, the priority is to protect the wound and promote healing. Offloading techniques, specialized dressings, and close monitoring reduce the risk of infection and prevent complications.
Managing swelling
Swelling is common after transmetatarsal amputations. Elevation, gentle compression, and controlled movement help decrease inflammation and support tissue recovery.
Maintaining mobility in surrounding joints
While the foot is healing, it is important to maintain mobility in the ankle, knee, and hip. Early movement prevents stiffness and prepares the body for rehabilitation.
Monitoring overall health conditions
Individuals who undergo transmetatarsal amputations often have underlying health conditions such as diabetes or vascular disease. Managing these conditions is essential for proper healing.
How Transmetatarsal Amputations Affect Mobility
Influence on gait patterns
Removal of the forefoot alters the mechanics of walking. The push off phase of gait is reduced because the toes and metatarsal heads are no longer present. This can cause shorter steps and changes in the timing of movement.
Changes in balance
The forefoot contributes significantly to balance, especially during forward movement and directional changes. Without this portion of the foot, individuals rely more heavily on the midfoot and heel.
Altered pressure distribution
Pressure shifts from the front of the foot to the back. This may increase stress on the heel and remaining structures. Proper footwear and orthotic design help reduce pressure concentrations.
Influence on speed and endurance
Walking may initially feel slower and require more effort. With training, strength conditioning, and adaptive equipment, many individuals regain mobility and improve their endurance.
Rehabilitation After Transmetatarsal Amputations
The importance of structured therapy
Rehabilitation is central to restoring independence. Therapists help individuals rebuild strength, improve balance, and relearn movement patterns that support safe mobility.
Strengthening surrounding muscles
Strengthening the calf muscles, ankle stabilizers, and hip muscles helps compensate for the loss of the forefoot. This increased support improves gait stability.
Balance retraining
Because the forefoot contributes to forward balance, therapy includes activities that retrain the body to distribute weight evenly and maintain stability during movement.
Gait training
Therapists teach individuals how to walk safely while maximizing the function of the remaining foot. This training includes step length adjustment, posture improvement, and movement coordination.
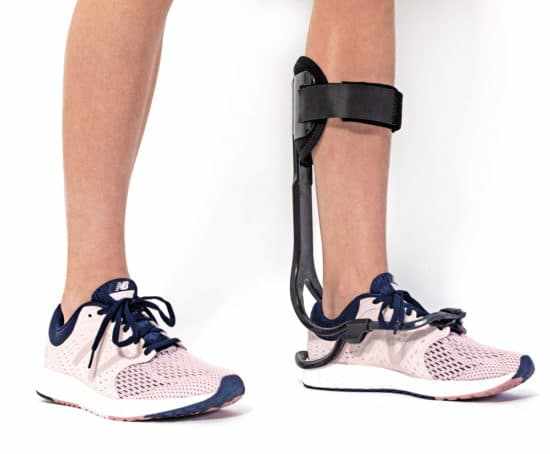
The Role of Footwear and Orthotic Devices
Supporting functional alignment
Custom footwear and orthotic inserts help distribute weight across the foot and compensate for the missing forefoot. Proper alignment improves comfort and walking efficiency.
Using partial foot prostheses
Partial foot prostheses restore some of the lost length and help individuals regain a more natural walking pattern. These devices can extend from the residual foot and provide a lever arm for push off.
Reducing pressure on sensitive areas
Cushioned insoles and supportive footwear help reduce pressure points on the heel and midfoot. This prevents skin breakdown and discomfort.
Enhancing stability
Orthotic devices that cradle the foot improve stability during walking and standing. These supports can reduce the risk of falls and improve overall mobility.
Long Term Considerations for Daily Living
Maintaining skin and tissue health
After a transmetatarsal amputation, regular skin checks become essential. Reduced sensation or changes in pressure distribution increase the risk of skin irritation or ulcers.
The importance of proper hygiene
Keeping the residual foot clean and dry prevents infections. Individuals are encouraged to monitor for redness, swelling, or wounds.
Ongoing medical follow up
Routine follow up with healthcare professionals helps ensure that footwear, prosthetic devices, and treatment plans continue to support mobility.
Adapting daily tasks
Most individuals adapt well to daily activities but may require minor modifications. These adjustments help maintain independence and comfort.
Psychological and Emotional Well Being
Adjusting to physical changes
Transmetatarsal amputations can affect self perception and confidence. Emotional support from family, friends, and mental health professionals plays an important role in recovery.
Celebrating progress
Focusing on small improvements encourages motivation. Each step toward greater independence contributes to emotional well being.
Staying engaged in meaningful activities
Remaining active and participating in enjoyable activities helps individuals maintain a sense of purpose and connection.
Improving Quality of Life Through Adaptive Strategies
Engaging in appropriate physical activities
Low impact activities such as cycling, swimming, and controlled walking help maintain fitness without placing excessive strain on the residual foot.
Using supportive devices
Canes, walkers, or trekking poles can offer additional support during specific activities. These tools help individuals feel more confident while moving.
Incorporating strength and flexibility exercises
Consistent exercise improves overall mobility, reduces fatigue, and supports long term health.
Conclusion
Transmetatarsal amputations present unique challenges, but with proper care, thoughtful rehabilitation, and the right supportive devices, individuals can regain meaningful mobility and independence. Understanding the procedure and its impact allows people to prepare both physically and emotionally for the recovery journey. Through dedication and comprehensive support, many individuals achieve a high quality of life and return to valued activities. This article is provided by Lermagazine.











Write a comment ...