
Charcot neuroarthropathy is a progressive and debilitating condition that affects the bones, joints, and soft tissues of the foot and ankle. It most commonly develops in individuals with peripheral neuropathy, particularly those with diabetes. Due to loss of protective sensation, patients may continue weight bearing despite ongoing injury, leading to bone fragmentation, joint collapse, and severe deformity. If not addressed appropriately, Charcot neuroarthropathy can result in chronic ulceration, infection, and limb loss.
Managing this condition requires a comprehensive and individualized treatment strategy that may include both surgical and non surgical approaches. In recent years, advancements in biomechanical assessment tools, particularly plantar pressure sensors, have significantly improved clinical understanding and management of Charcot neuroarthropathy. These tools provide valuable insights into pressure distribution and gait patterns, helping guide treatment decisions and improve outcomes.
Understanding Charcot Neuroarthropathy
Disease Mechanism and Progression
Charcot neuroarthropathy develops as a result of impaired sensation combined with repetitive mechanical stress. Loss of pain perception allows microtrauma to go unnoticed, while continued ambulation accelerates bone and joint destruction. Increased blood flow to the affected area further weakens bone structure, increasing susceptibility to fractures and collapse.
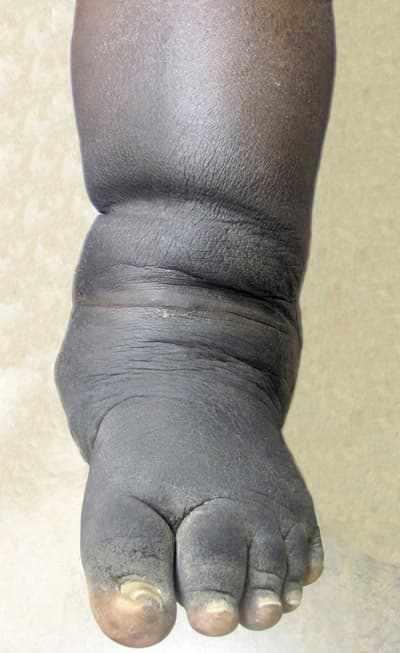
As the condition progresses, structural deformities alter foot biomechanics. These changes lead to abnormal pressure distribution across the plantar surface, increasing the risk of skin breakdown and ulcer formation. Understanding these biomechanical shifts is critical for effective treatment planning.
Clinical Stages of the Condition
The condition typically progresses through an acute inflammatory stage, a subacute reparative stage, and a chronic consolidation stage. Early identification during the acute phase offers the best opportunity to prevent severe deformity. Once the chronic stage is reached, permanent structural changes are often present, requiring more complex management.
Goals of Treatment in Charcot Neuroarthropathy
Preserving Foot Structure and Function
The primary goal of treatment is to maintain or restore a stable, plantigrade foot capable of safe weight bearing. Preventing collapse and maintaining alignment helps preserve mobility and independence.
Reducing Plantar Pressure and Injury Risk
Abnormal pressure concentration plays a central role in ulcer development. Effective treatment focuses on redistributing plantar pressure to minimize stress on vulnerable areas.
Preventing Long Term Complications
Avoiding ulceration, infection, and amputation is essential. Both surgical and non surgical approaches aim to reduce repetitive trauma and improve mechanical stability.
Non Surgical Approaches to Charcot Neuroarthropathy
Immobilization and Offloading
Immobilization is the foundation of non surgical management, particularly during the acute stage. Total contact casting or removable immobilization devices are used to limit motion and reduce mechanical stress. Strict offloading allows inflammation to subside and fractures to heal.
Patient adherence to offloading protocols is critical. Inadequate immobilization can accelerate disease progression and worsen deformity.
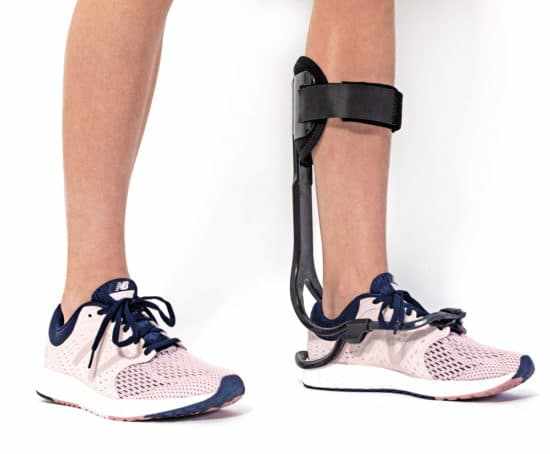
Role of Custom Orthoses and Footwear
Once acute inflammation resolves, patients transition to custom orthoses and therapeutic footwear. These devices are designed to accommodate deformities and redistribute pressure across the foot. Proper customization is essential to prevent localized stress that can lead to ulceration.
Importance of Plantar Pressure Sensors in Conservative Care
Plantar pressure sensors have become an invaluable tool in non surgical management. These devices measure pressure distribution across the plantar surface during standing and walking. By identifying high pressure areas, clinicians can adjust orthoses and footwear to reduce risk.
In patients with Charcot neuroarthropathy, plantar pressure sensors help detect subtle biomechanical changes before visible injury occurs. Ongoing monitoring allows for timely intervention, reducing the likelihood of skin breakdown and recurrent trauma.
Patient Education and Monitoring
Education plays a vital role in conservative management. Patients must understand the importance of daily foot inspection, adherence to prescribed footwear, and early reporting of changes. Regular follow up appointments allow clinicians to reassess pressure distribution and adjust treatment as needed.
Indications for Surgical Intervention
Failure of Non Surgical Management
Surgery is considered when conservative measures fail to achieve a stable and functional foot. Persistent deformity, instability, or recurrent ulceration despite optimal offloading may necessitate operative intervention.
Severe Deformity and Structural Instability
Advanced Charcot neuroarthropathy can result in significant joint collapse and abnormal alignment. When deformities cannot be adequately accommodated with orthoses, surgical correction may be required to restore biomechanical balance.
Recurrent Ulceration Due to Pressure Points
Bony prominences created by deformity often lead to chronic ulceration. Surgical correction may be necessary to eliminate pressure points and reduce the risk of infection.
Surgical Approaches to Charcot Neuroarthropathy
Reconstructive Surgical Techniques
Reconstructive surgery aims to realign bones and stabilize joints. Procedures may include osteotomy, joint fusion, and internal fixation. The objective is to create a foot structure that distributes plantar pressure evenly and supports functional ambulation.
Arthrodesis for Long Term Stability
Joint fusion is commonly used to address severe instability. By eliminating abnormal joint motion, arthrodesis provides long term stability and reduces the risk of recurrent deformity. Healing requires prolonged immobilization and careful postoperative management.
Exostectomy for Targeted Pressure Relief
In selected cases, removal of bony prominences may be sufficient to relieve localized pressure and promote ulcer healing. This approach is less invasive than full reconstruction and may be appropriate for patients with stable deformities.
Postoperative Rehabilitation and Assessment
Postoperative care involves strict non weight bearing followed by gradual reintroduction of activity. Plantar pressure sensors can play a critical role during rehabilitation by evaluating pressure distribution as patients return to ambulation. This data helps guide orthotic adjustments and ensures safe loading patterns.
Comparing Surgical and Non Surgical Approaches
Benefits of Non Surgical Treatment
Non surgical management avoids operative risks and is highly effective when initiated early. It emphasizes preservation of existing anatomy and prevention of disease progression.
Benefits of Surgical Treatment
Surgical intervention provides definitive correction for advanced deformities. When successful, it can significantly reduce ulcer recurrence, improve alignment, and enhance long term mobility.
Risks and Limitations of Each Approach
Conservative treatment requires prolonged immobilization and high patient compliance. Surgical treatment carries risks such as infection, delayed healing, and hardware complications. Treatment decisions must be individualized based on patient health, disease severity, and functional goals.
Long Term Management and Follow Up
Ongoing Surveillance and Risk Reduction
Charcot neuroarthropathy is a chronic condition that requires lifelong monitoring. Even after successful treatment, patients remain at risk for recurrence or new areas of pressure overload.
Continued Use of Plantar Pressure Sensors
Plantar pressure sensors support long term management by providing objective data on gait and load distribution. Regular assessments help identify emerging risk areas and guide preventive interventions.
Multidisciplinary Approach to Care
Optimal outcomes are achieved through collaboration among healthcare professionals specializing in foot and ankle care, metabolic disease management, rehabilitation, and wound prevention. Addressing both biomechanical and systemic factors is essential for sustained success.
Conclusion
Surgical and non surgical approaches to Charcot neuroarthropathy each play a vital role in managing this complex and potentially limb threatening condition. Early diagnosis and prompt conservative care can slow progression and preserve foot structure. In advanced cases, surgical intervention offers an opportunity to restore stability and prevent serious complications.
The integration of plantar pressure sensors has enhanced both treatment planning and long term management by providing critical insights into foot biomechanics. By guiding offloading strategies, orthotic design, and postoperative rehabilitation, these tools contribute to improved outcomes and reduced complication rates.
Successful management of Charcot neuroarthropathy requires individualized treatment, patient engagement, and ongoing monitoring. Through a balanced approach that combines clinical expertise with biomechanical assessment, long term limb preservation and functional mobility can be achieved.










Write a comment ...